Customer Rep Portal
2024–2025
I designed a standalone internal product for customer service customer reps supporting Medicare Prescription Payment Plan members, reducing average call time by 8% and replacing an impersonation-based workflow across Humana, Express Scripts, and Cigna that dropped time spent adding a payment method by ~42%.
Role
Founding Designer
Company
Paytient
Client
Humana
Express Scripts
Cigna
Shipped
Oct 2024
My role
I was the Founding Product Designer on this project to ship this work. I started alongside a Product Manager and Staff Engineer to build this product and the design system from the ground up in less than 10 months.
Context
The Medicare Prescription Payment Plan was a net-new federal program that allowed seniors on Part D to spread their out-of-pocket prescription costs over the calendar year instead of paying in full at the pharmacy.
Paytient stepped in to create a white-labeled product offering to support the end-to-end needs from this CRM portal for customer reps to use when supporting members, to a member portal and a calculator tool.
Problem
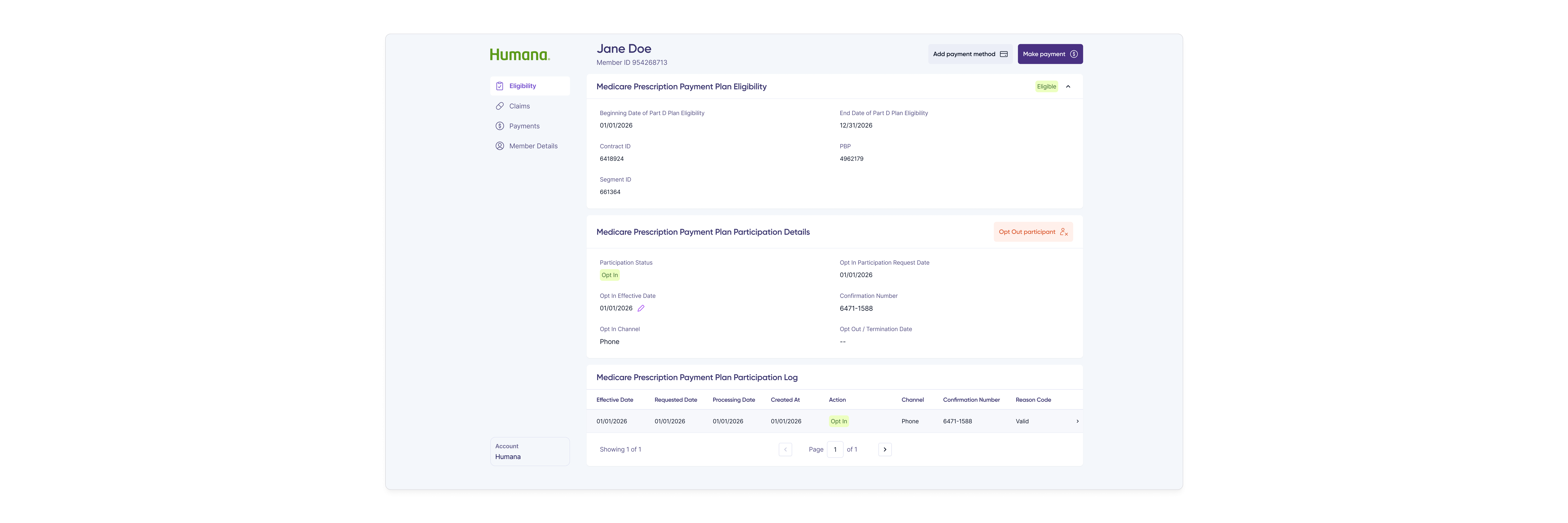
Customer reps were the humans on the other end of every call when a member needed support. The original model had them impersonating the member portal. When a call came in, the customer rep authenticated into that member's account and navigated the member-facing interface to guide the conversation. It was fast to build. It failed in several ways at once.
- The portal was designed for a senior managing her own account once a month, not an operator handling hundreds of accounts a day.
- Customer reps could only see what members could see, which meant no confirmation numbers, no opt-in channel, no reason codes, no eligibility dates.
- Authentication was its own tax: members often couldn't remember their login, and two minutes of credential recovery was a meaningful slice of a customer's time budget.
The support model needed to be rebuilt as its own product.
Trigger impersonation
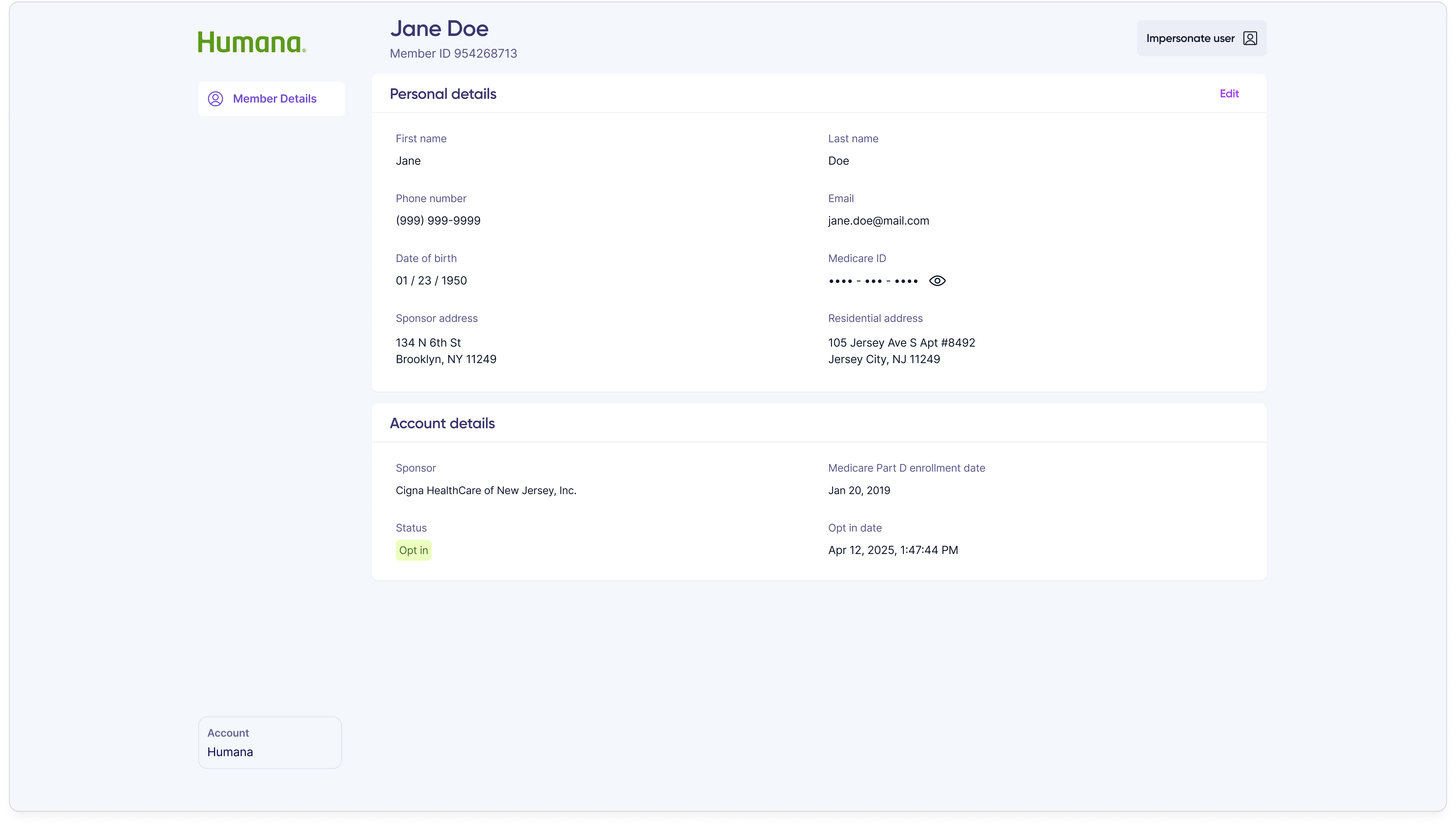
Confirm intent
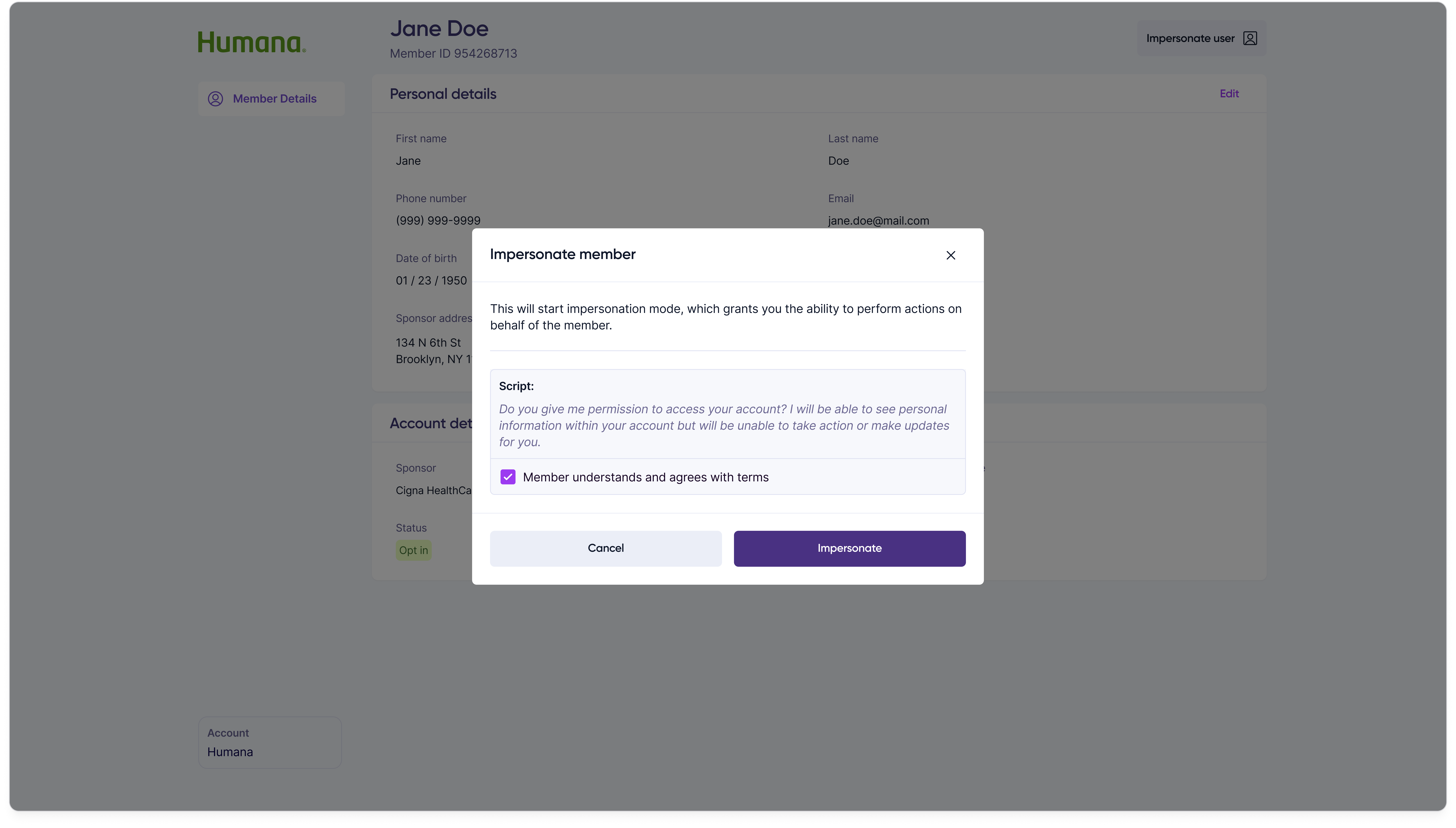
Loading
Customer rep impersonating member portal
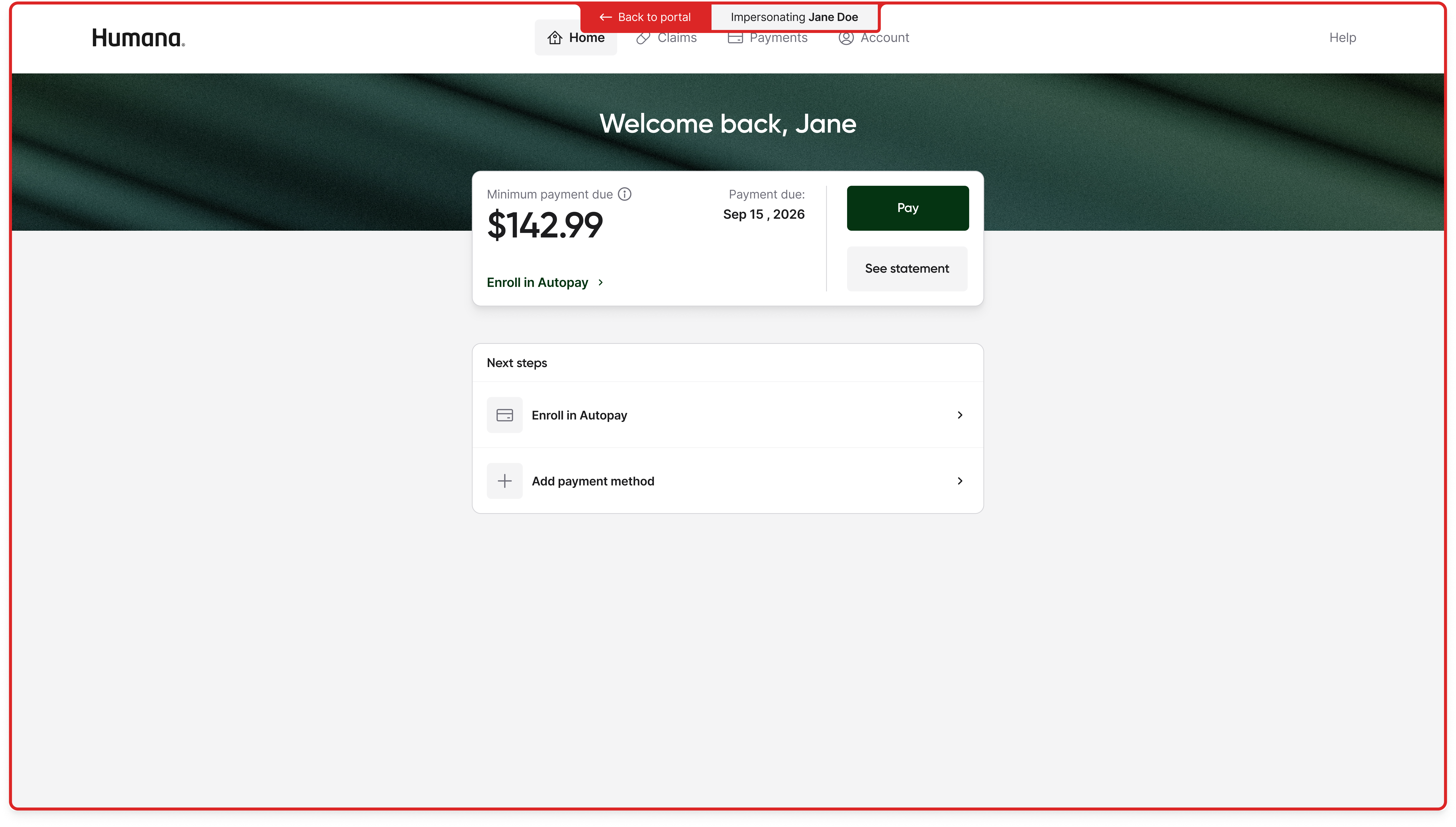
Process
I spent time with customer reps to understand the shape of a support call, the moments where impersonation failed, and the actions customer reps needed to take that the member's portal would not let them.
I structured the portal around the domains of information customer reps actually worked in, rather than around member-facing tasks. The member portal is organized around things a member does — home, claims, payments, account. The customer rep portal is organized around data domains an operator needs to pull from quickly.
Final designs
The shipped customer rep portal is a purpose-built internal product covering every action a customer rep takes during a support call, with the information density and direct-action capability that member-facing products are designed to avoid.
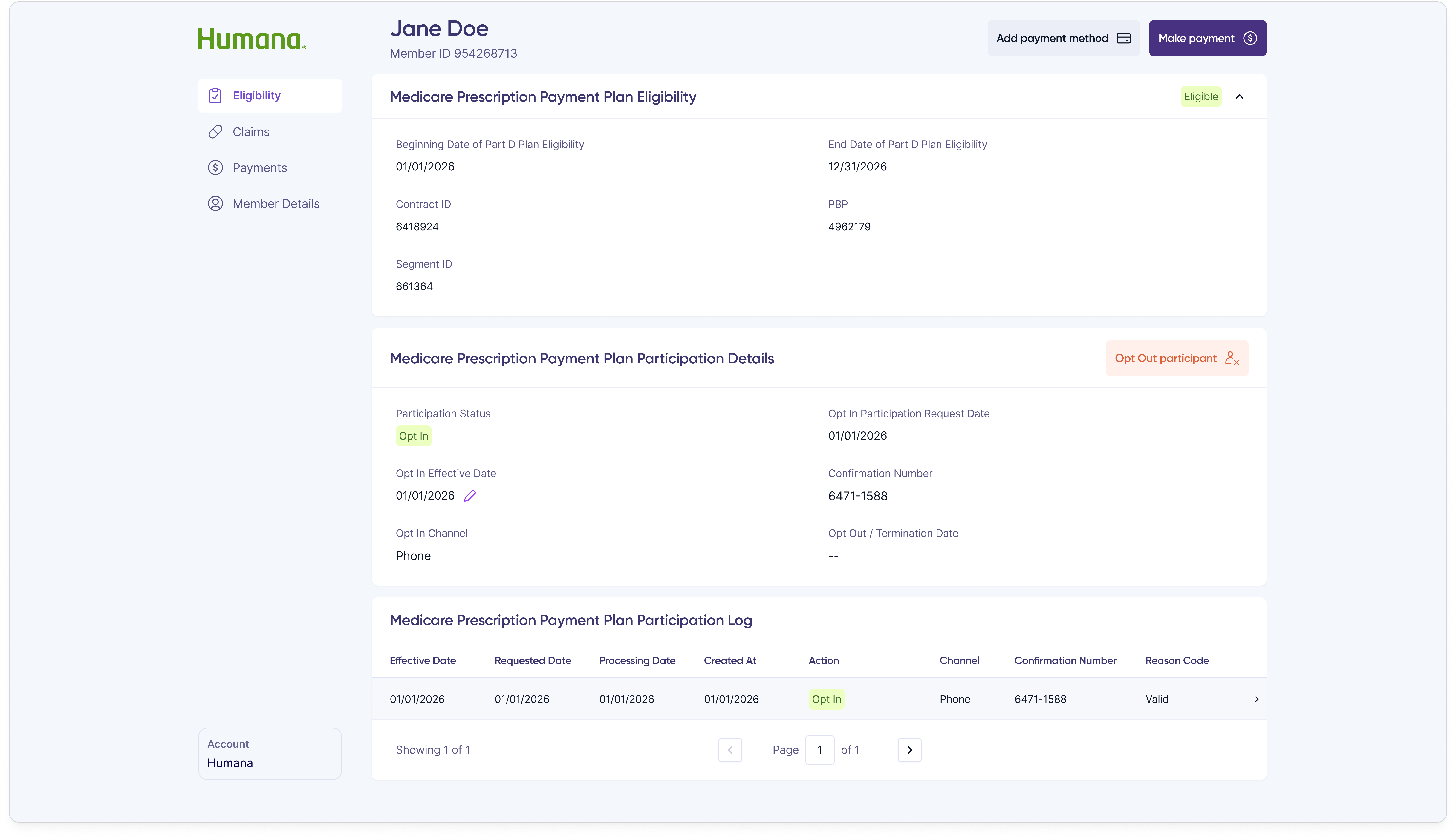
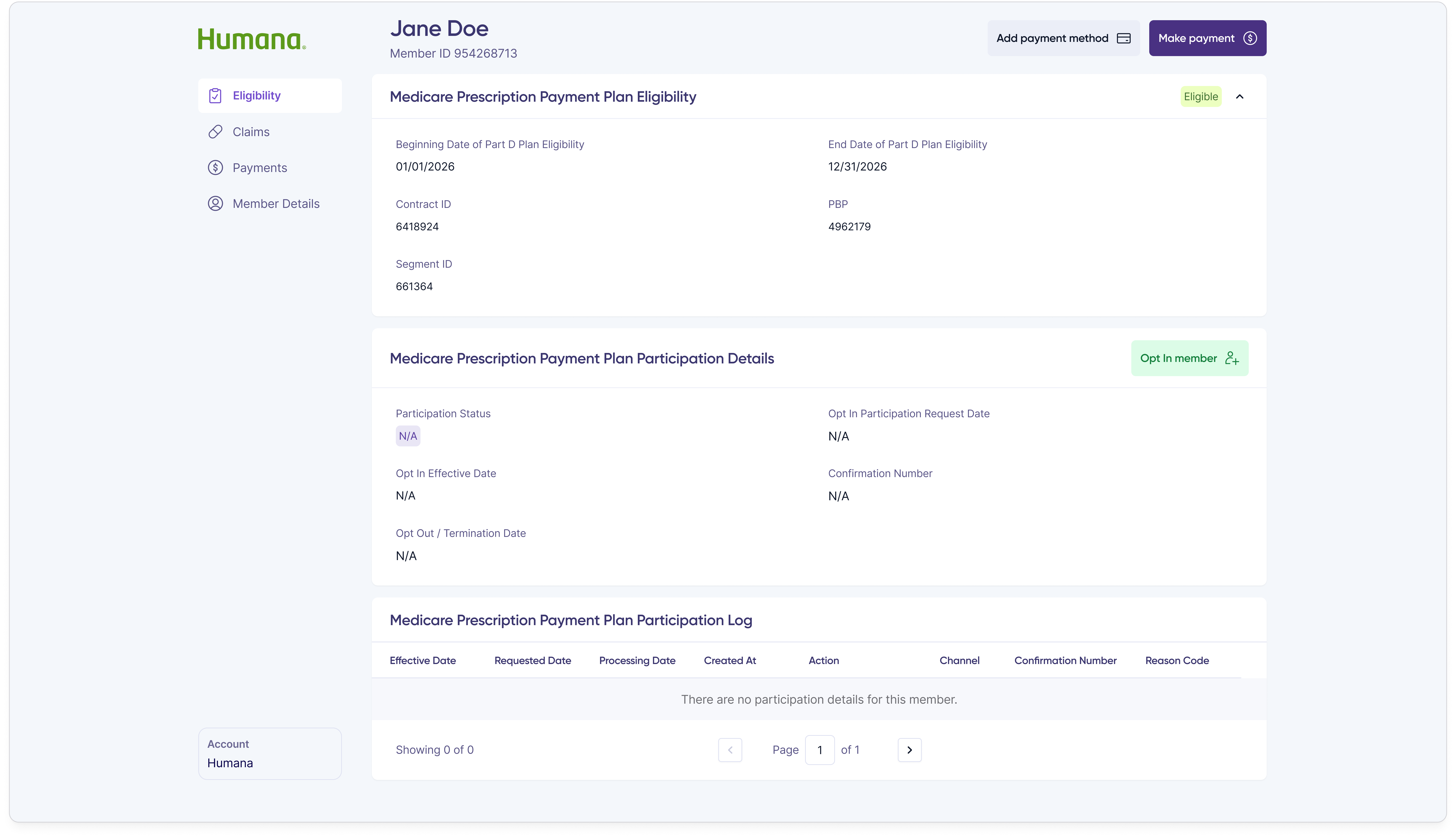
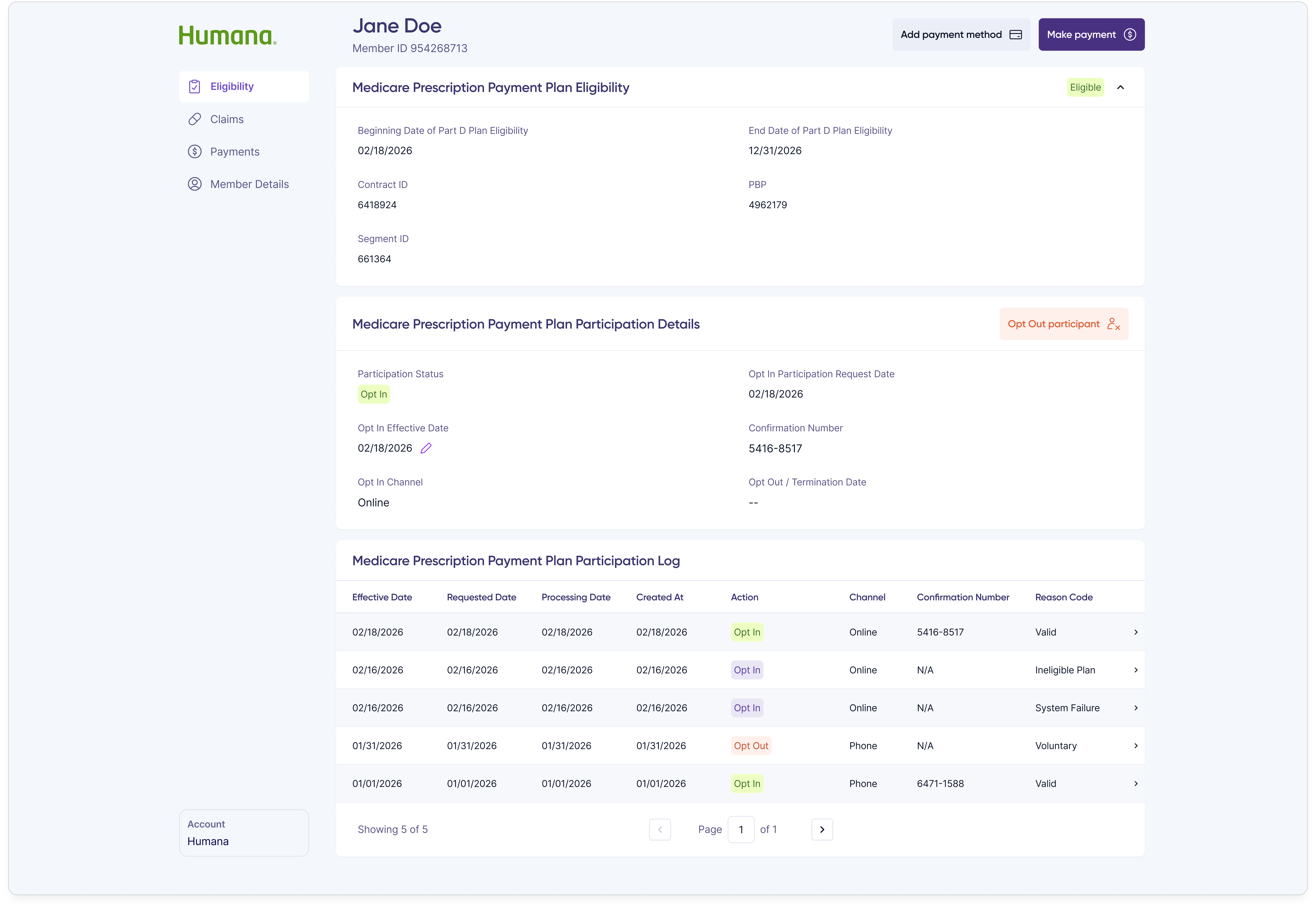
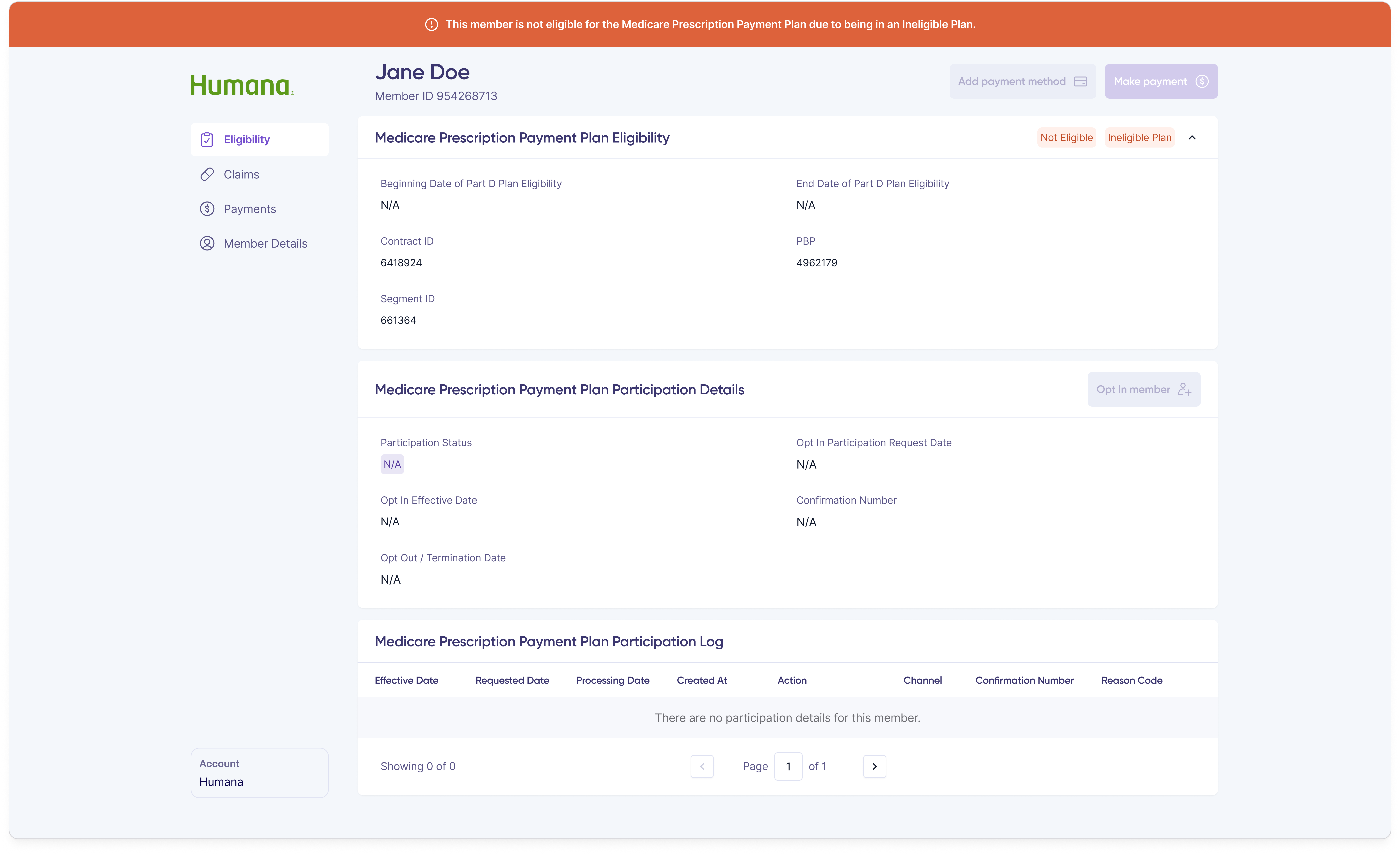
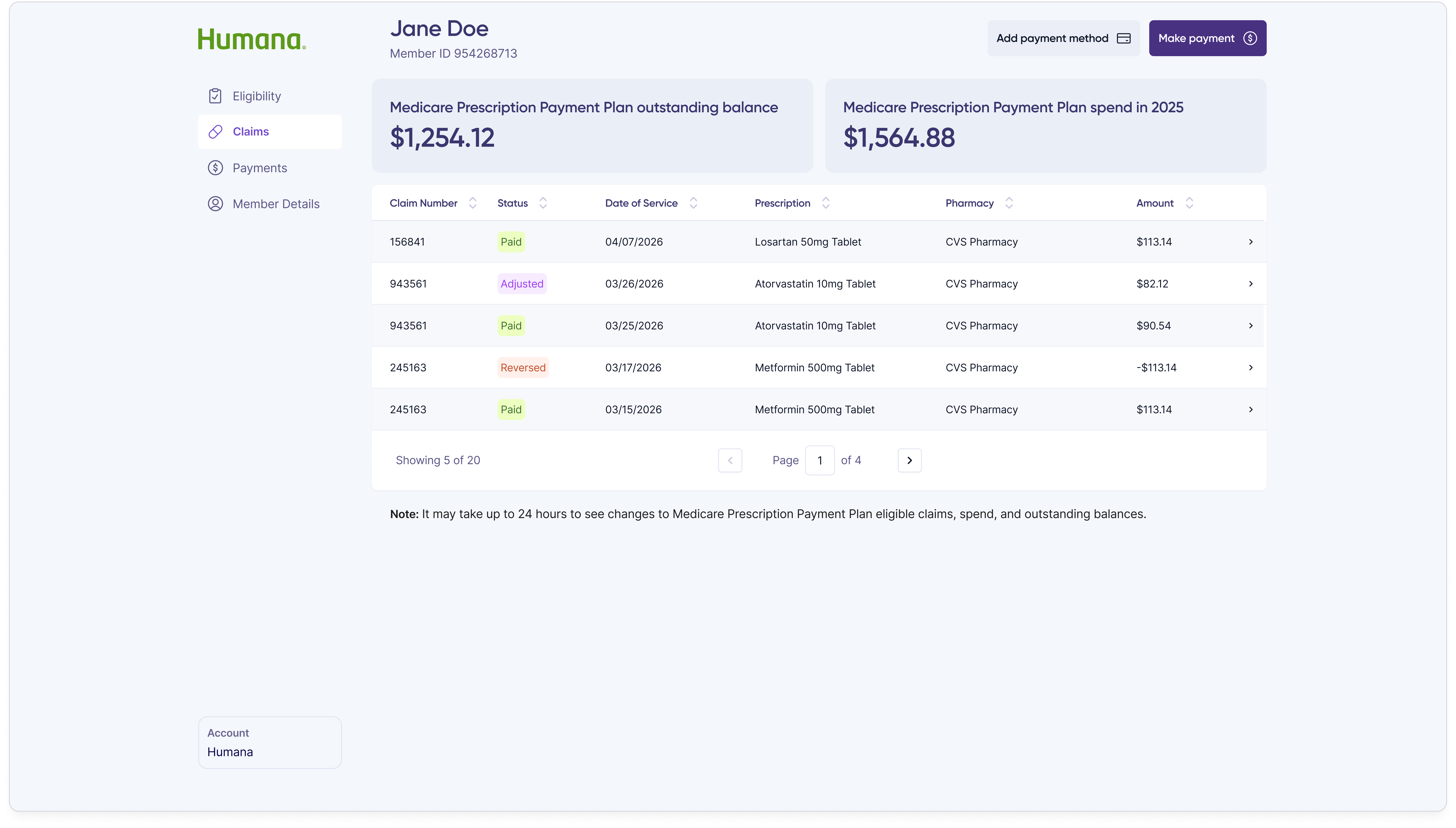
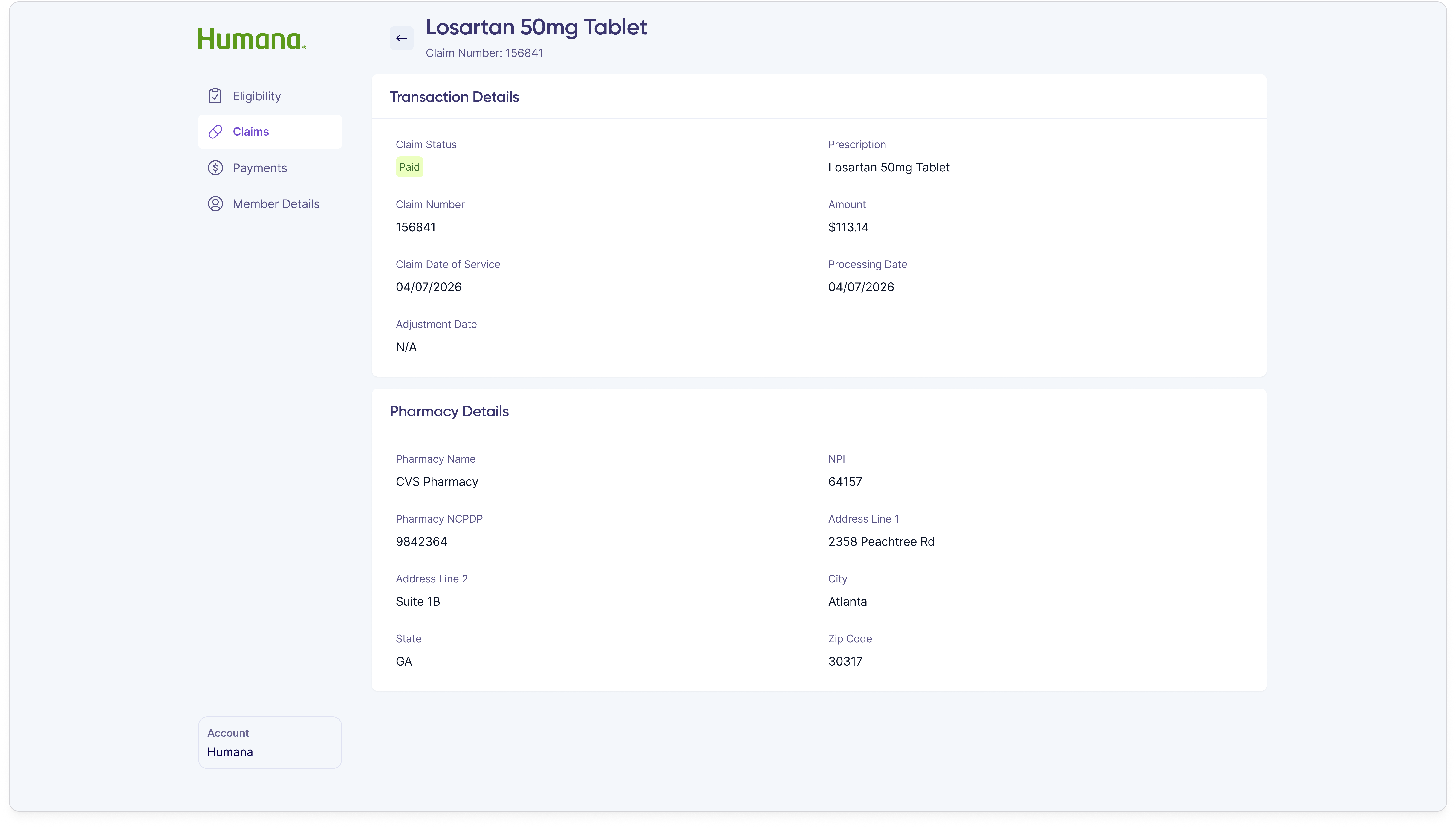
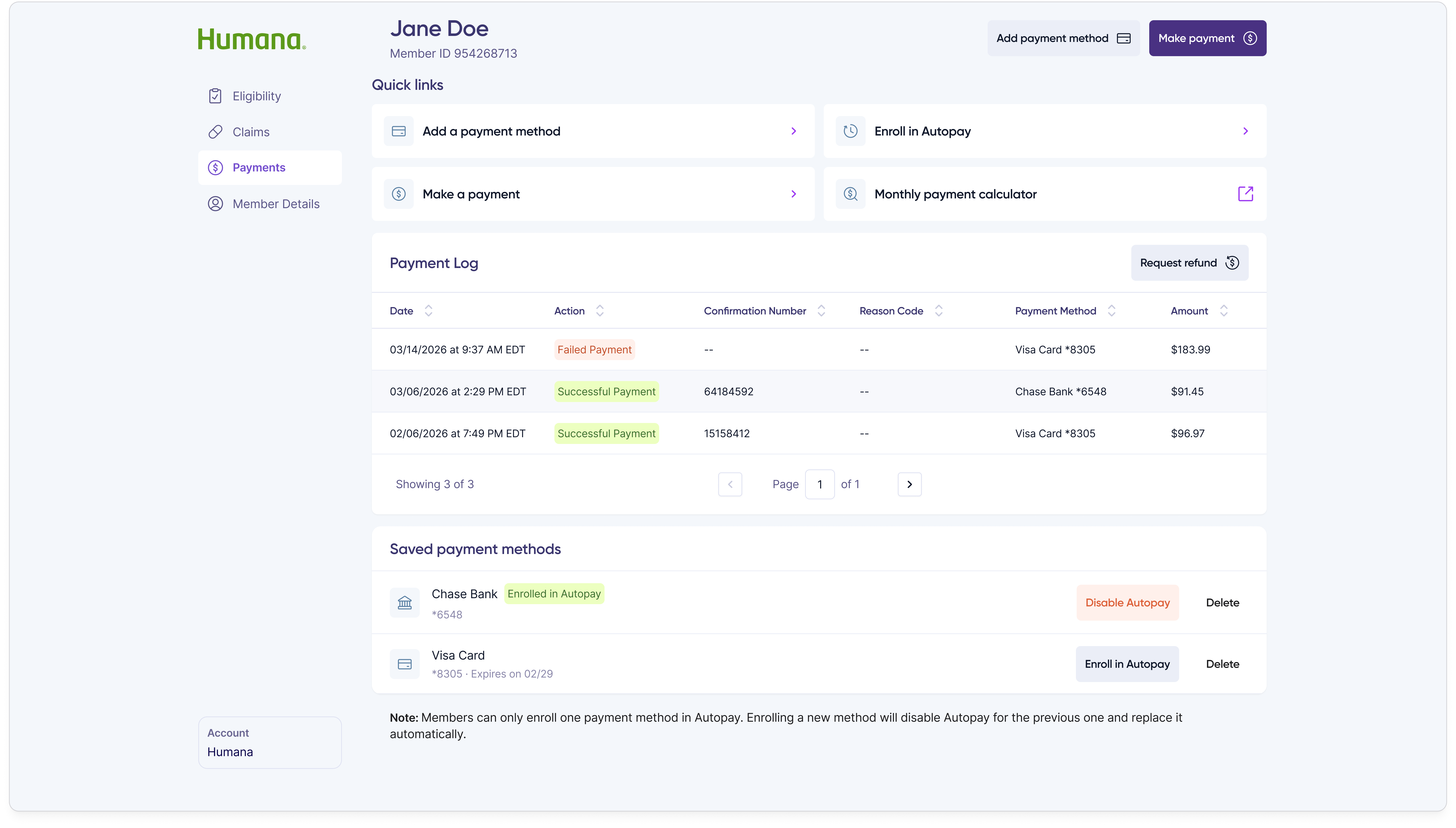
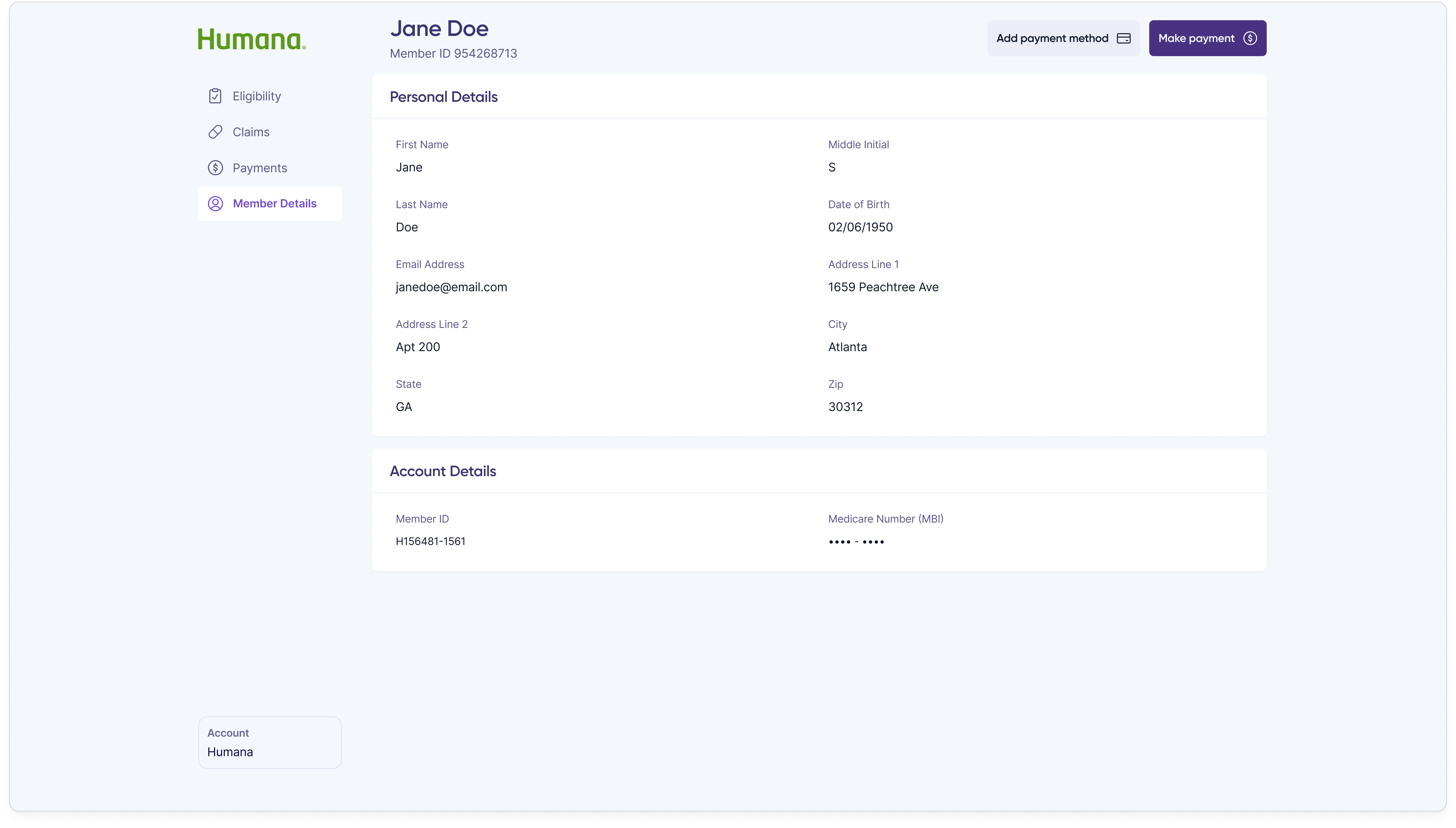
When a member overpaid or sent money to the wrong place, customer reps needed a way to resolve it without leaving the portal. The refund flow starts with a single modal that surfaces the overpayment amount and asks the customer rep to pick a request type.
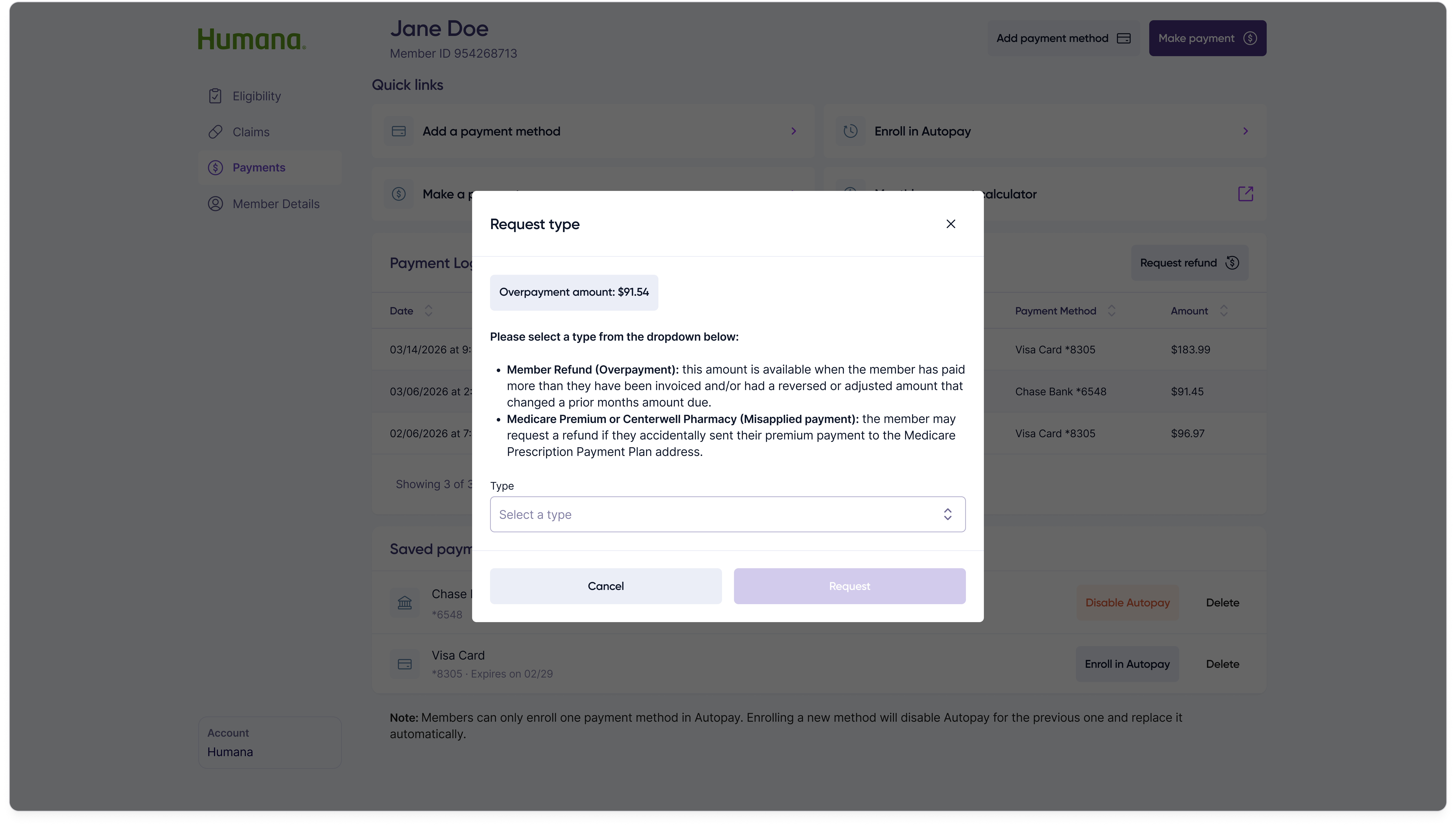
Selecting a request type swaps the modal contents into one of three sub-forms — refund the member, transfer the funds to a Medicare premium, or transfer them to the pharmacy — each collecting only the fields that specific resolution path requires.
Member refund
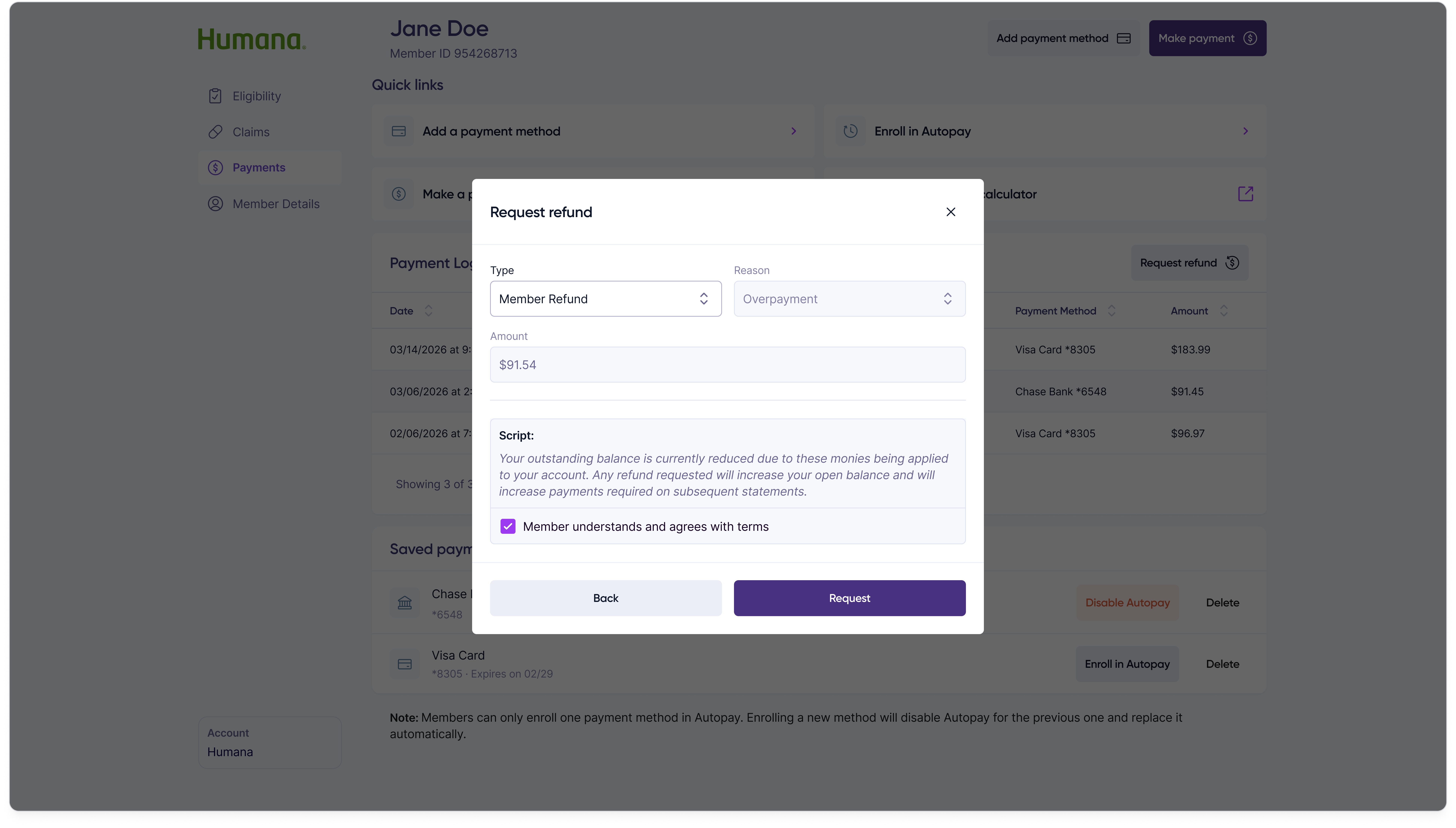
Transfer to Medicare premium
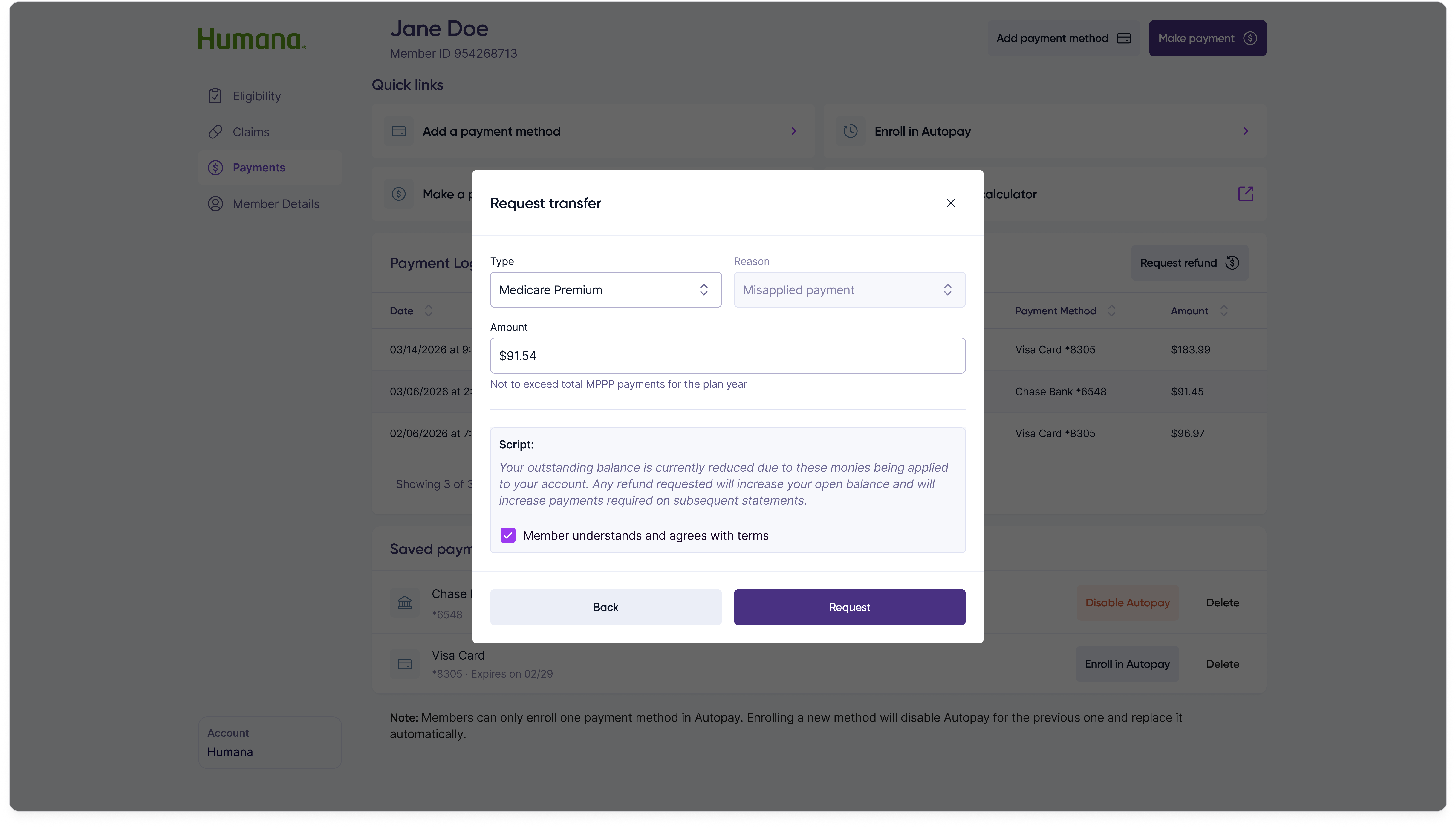
Transfer to pharmacy
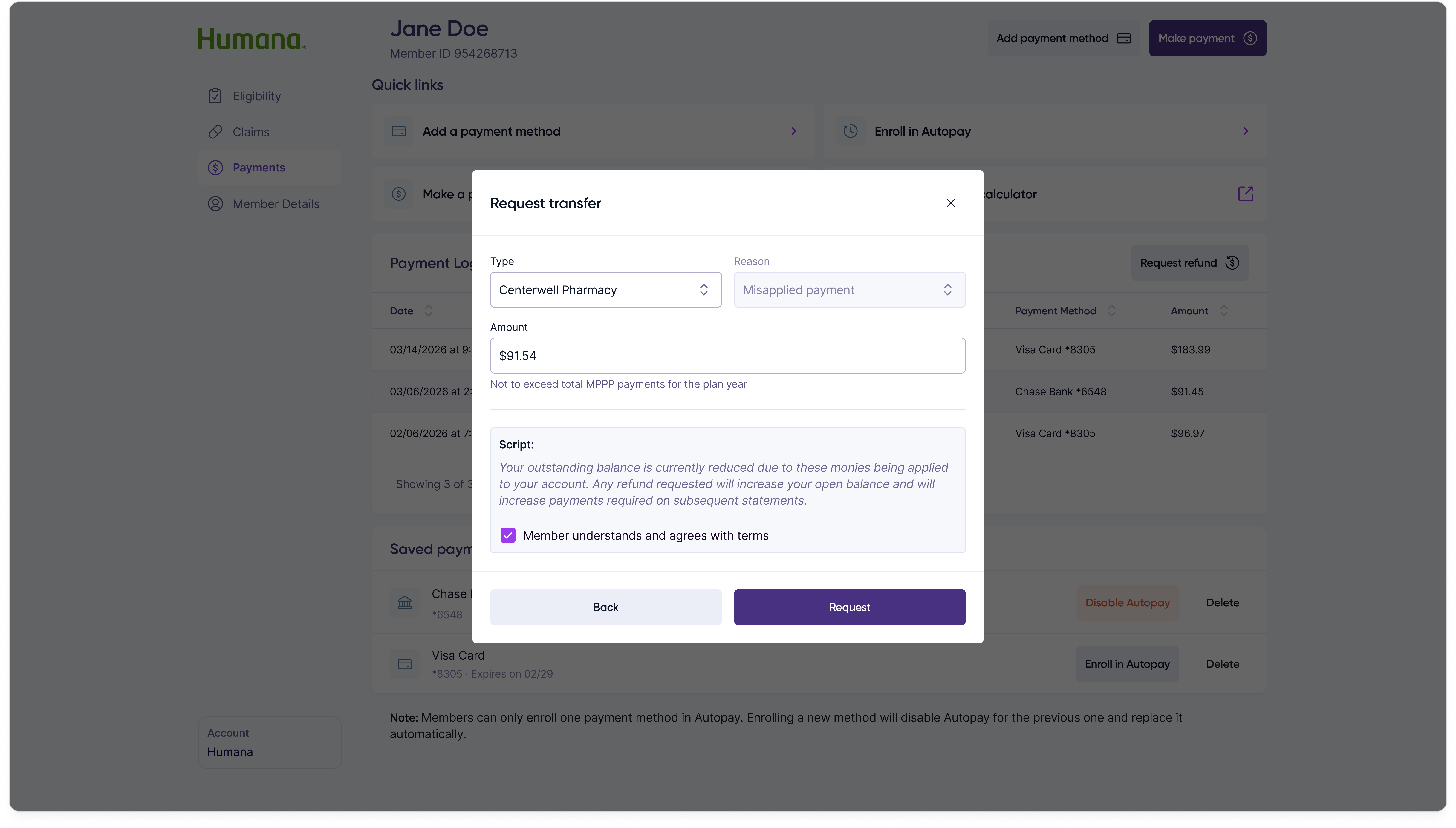
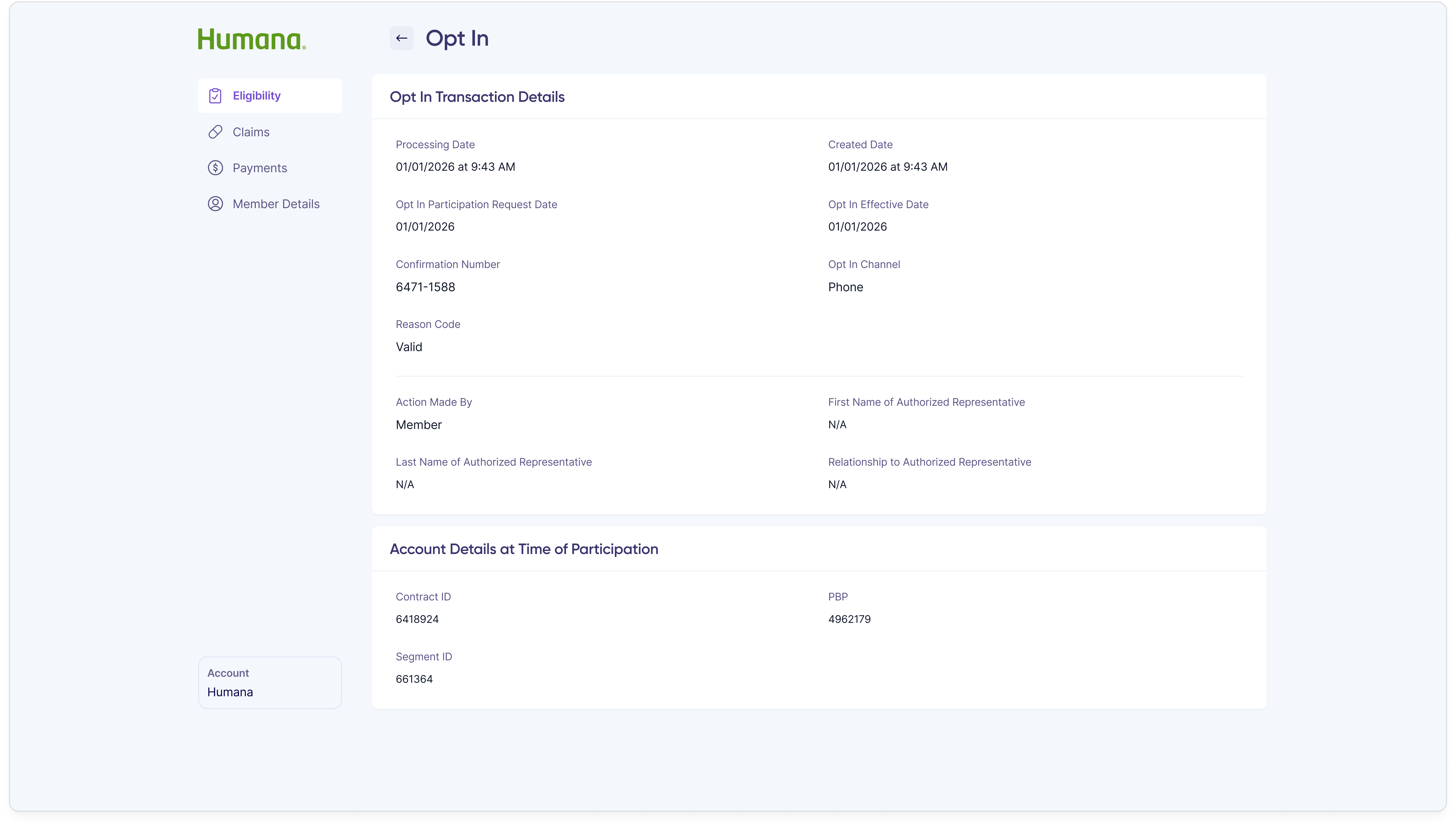
Opting a member into the program is the most consequential action a customer rep takes — it commits the member to spreading their out-of-pocket prescription costs across the plan year. The flow is two steps: capture authorization and channel, then confirm.
Step 1 — Authorization & details
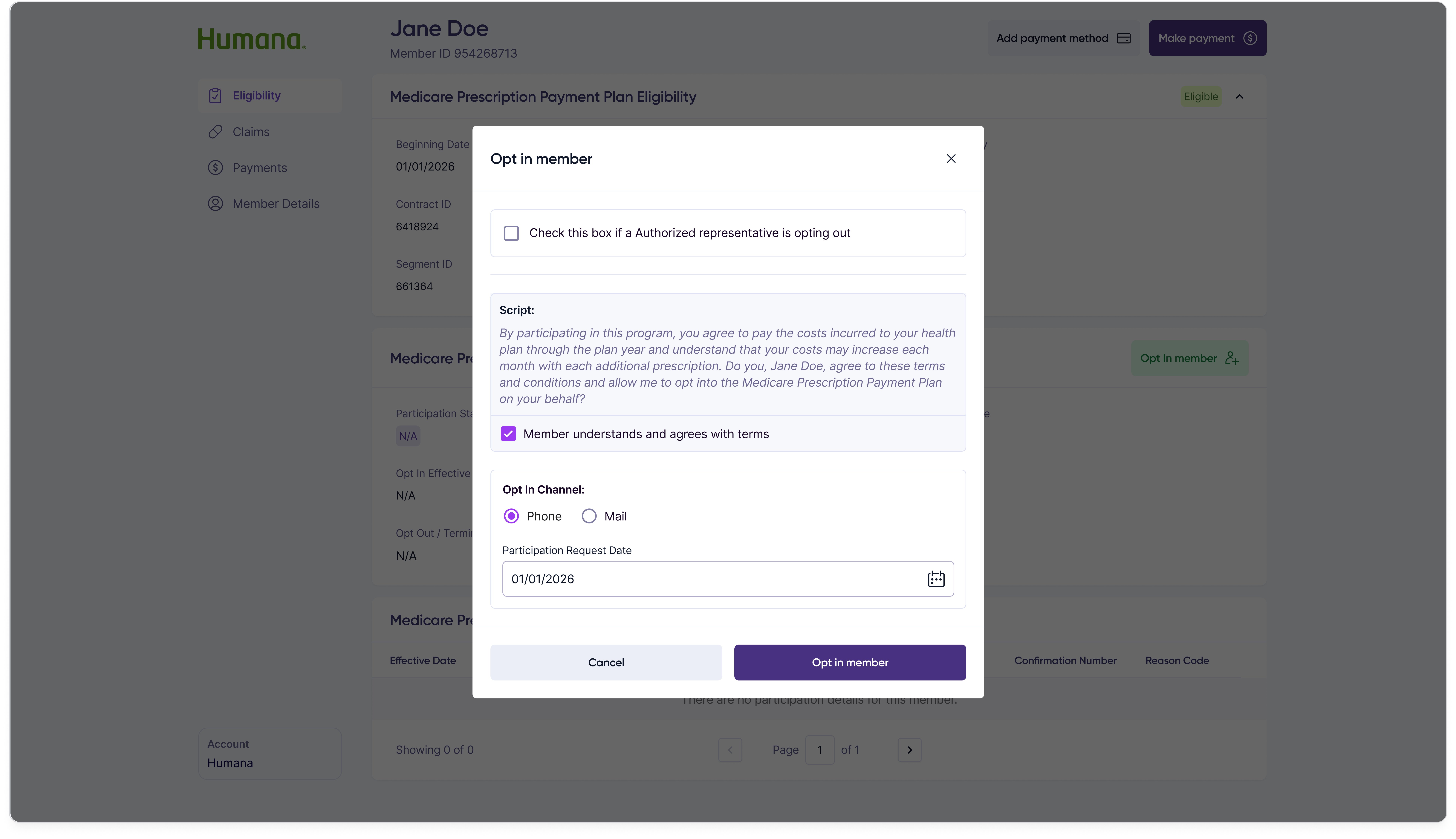
Step 2 — Confirmation
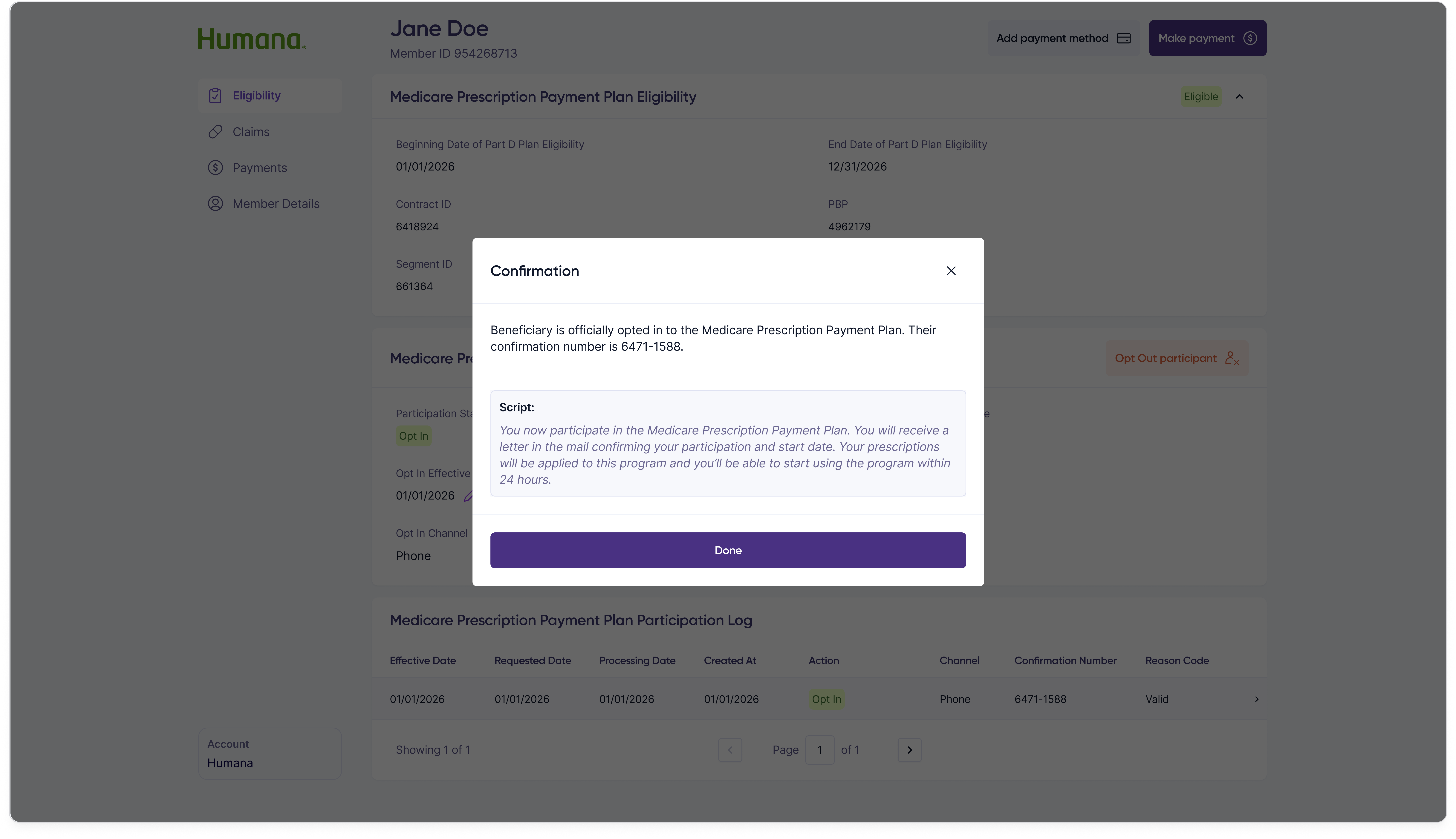
Opting out follows the same two-step shape so customer reps only have one mental model to learn for participation changes.
Step 1 — Reason & details
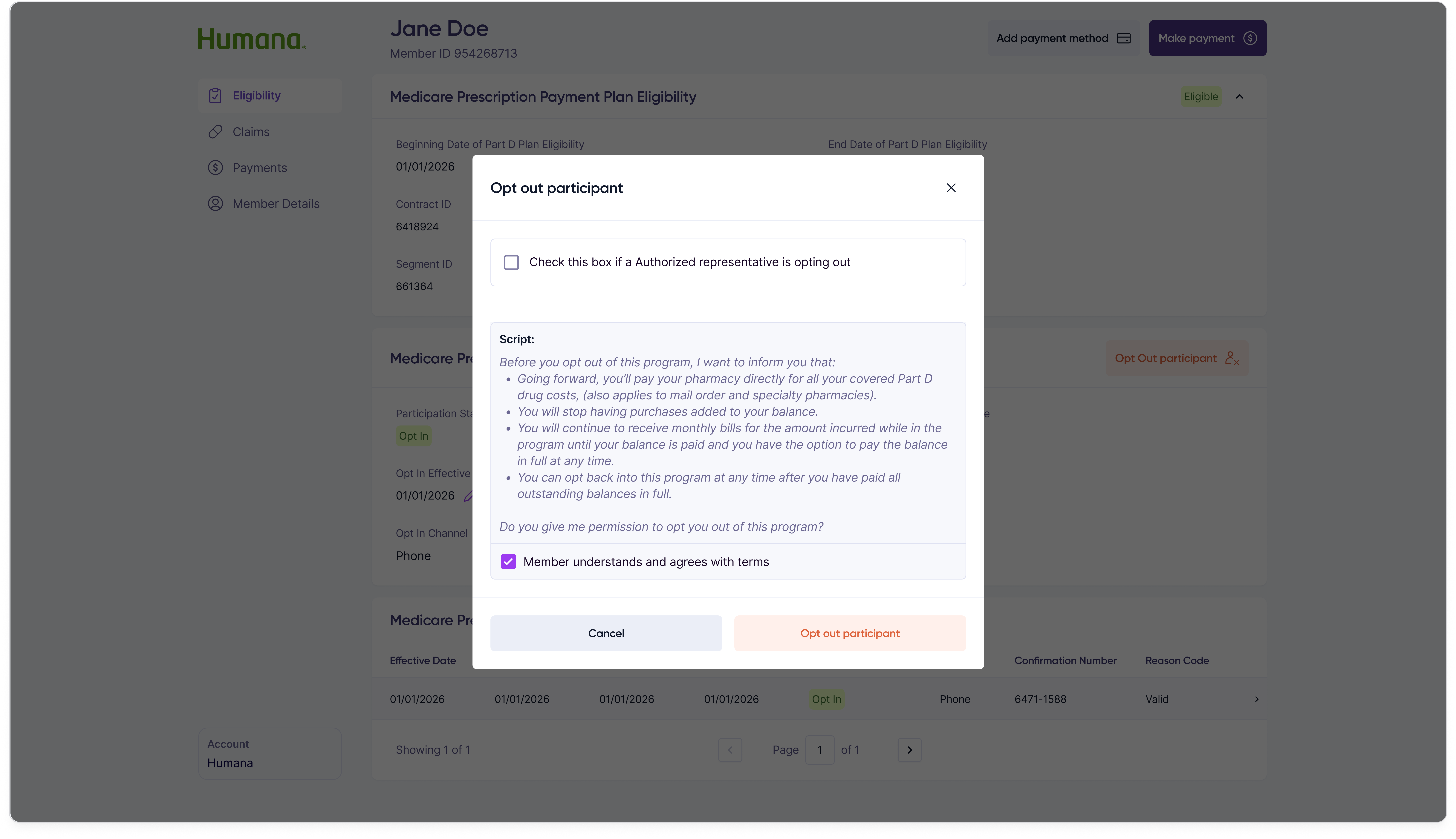
Step 2 — Confirmation
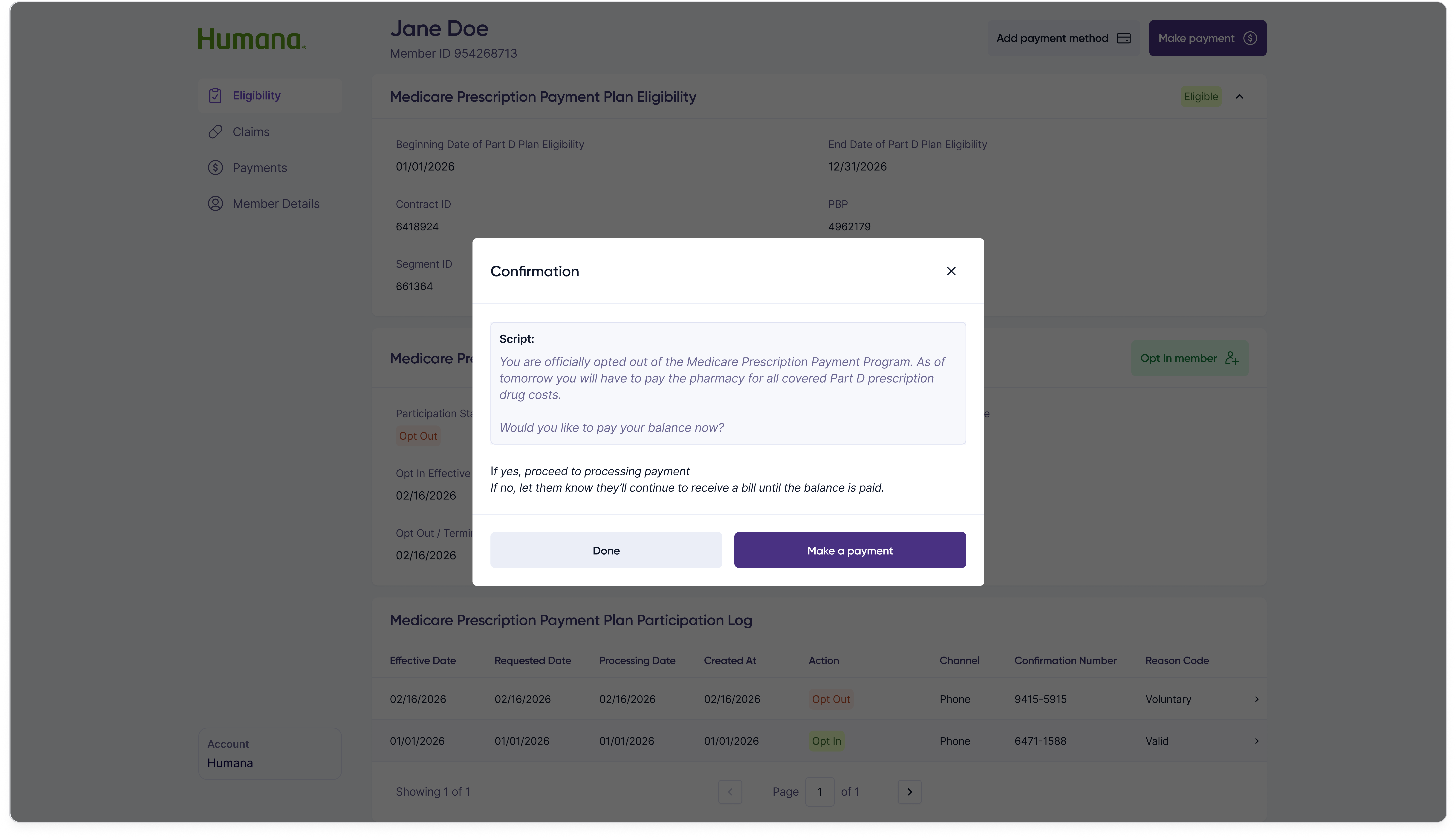
Opt-in effective dates occasionally need to be backdated when paperwork lags real-world events. Rather than re-running the full opt-in flow, customer reps can edit the date inline from the participation details panel.
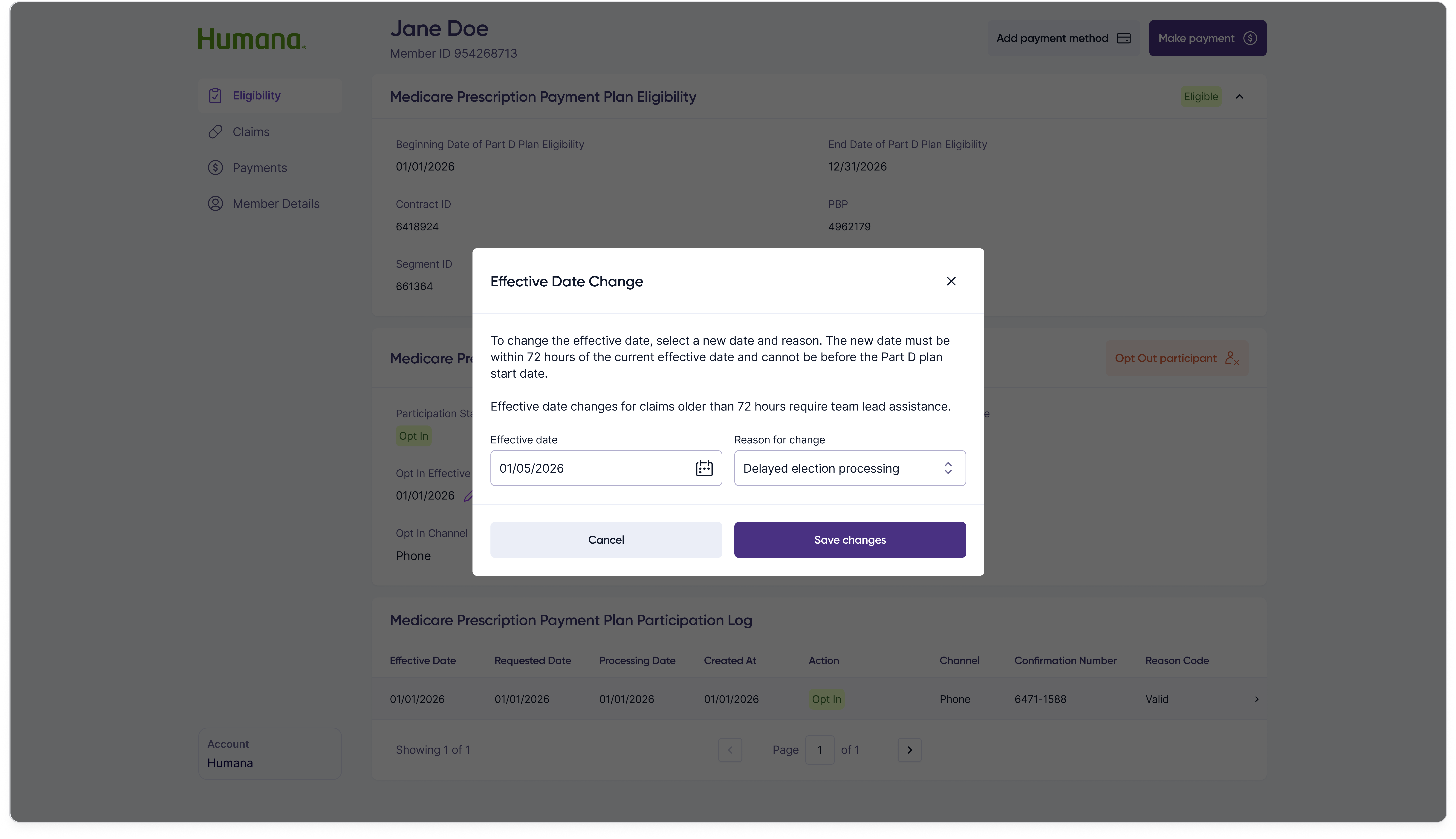
Taking a payment over the phone is the highest-volume action on the portal. The flow is four steps — choose amount, choose method, review, and confirm — each its own screen so the customer rep and member stay aligned at every commitment point.
Step 1 — Choose amount
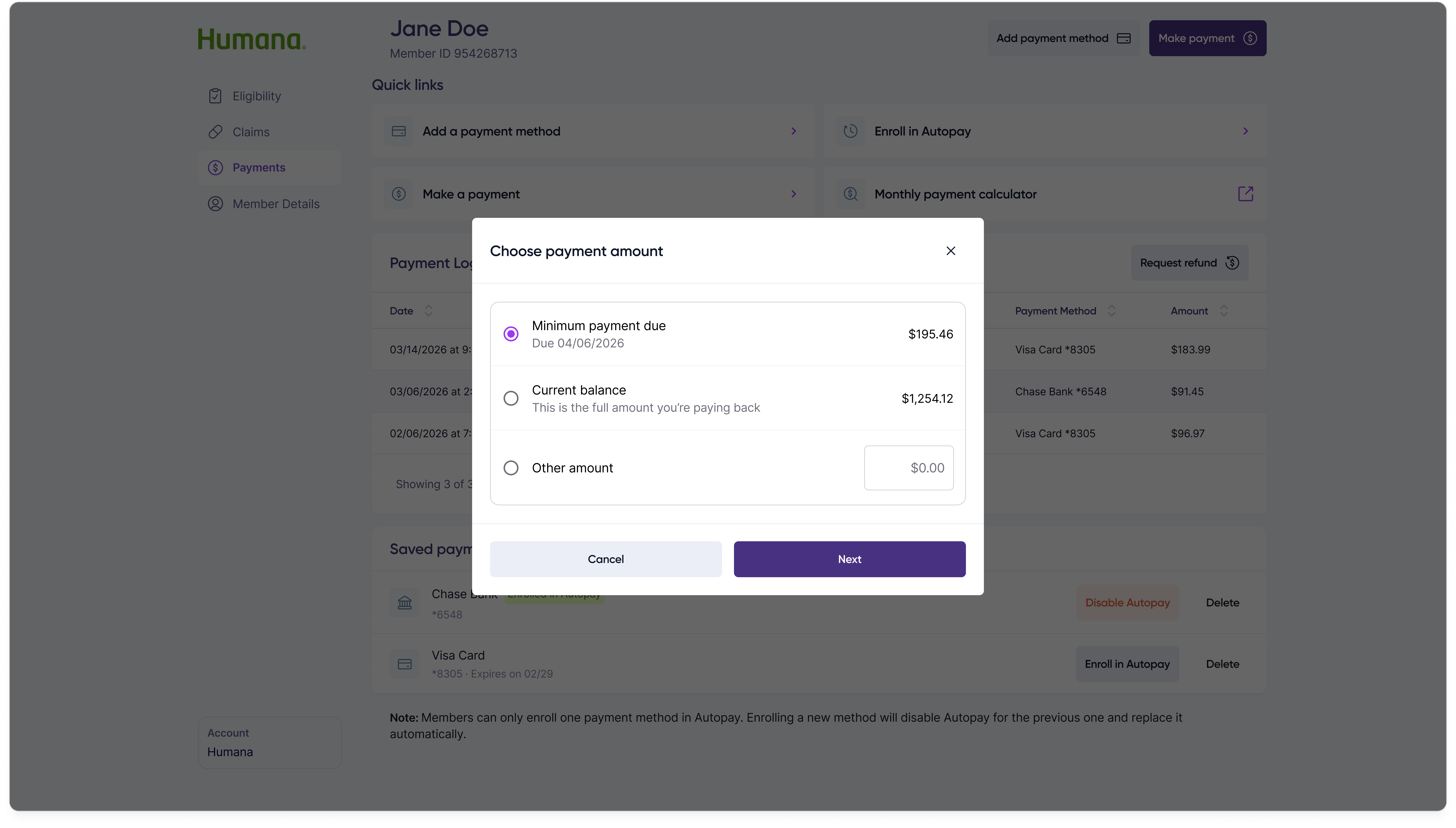
Step 2 — Choose method
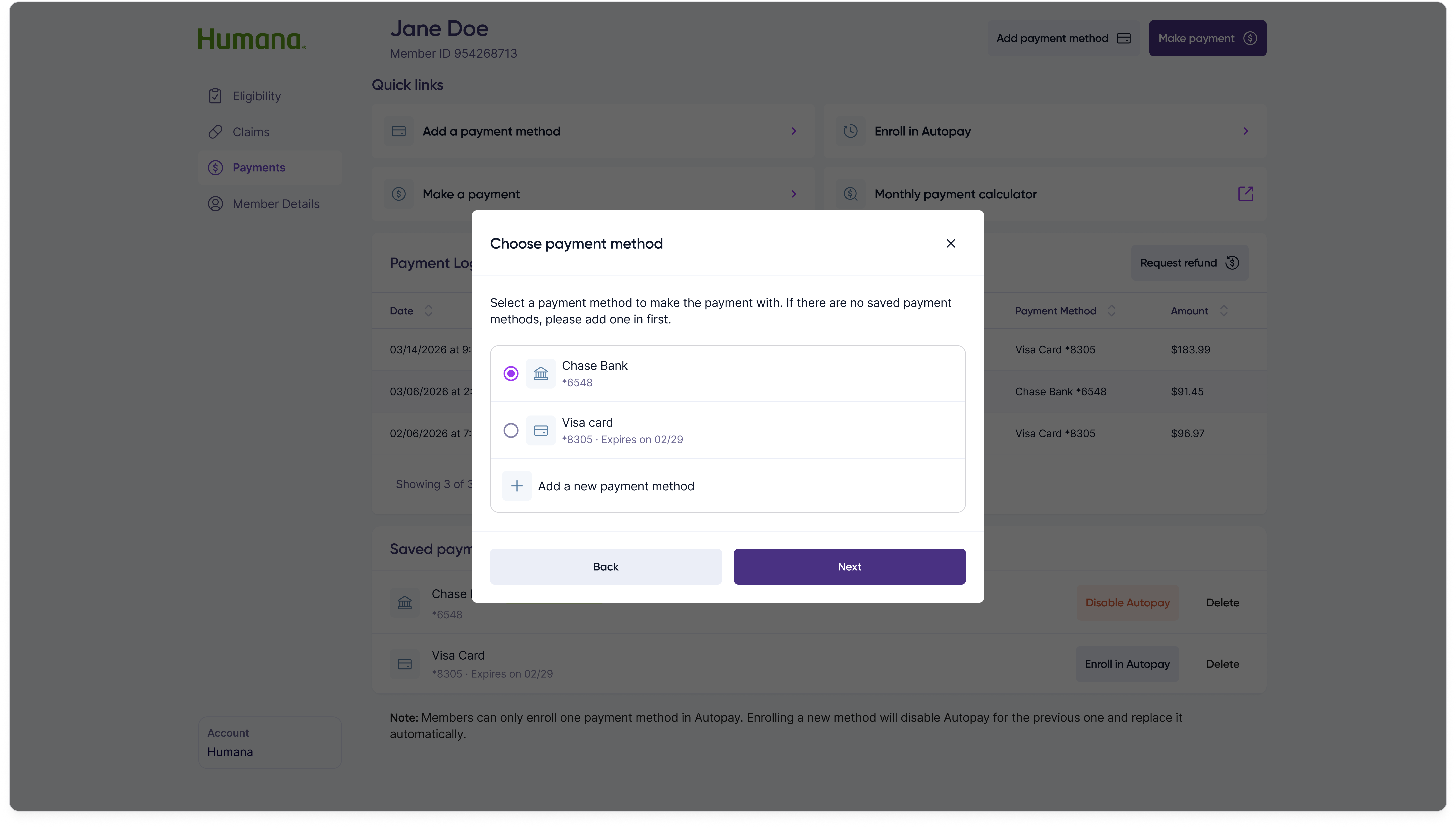
Step 3 — Review
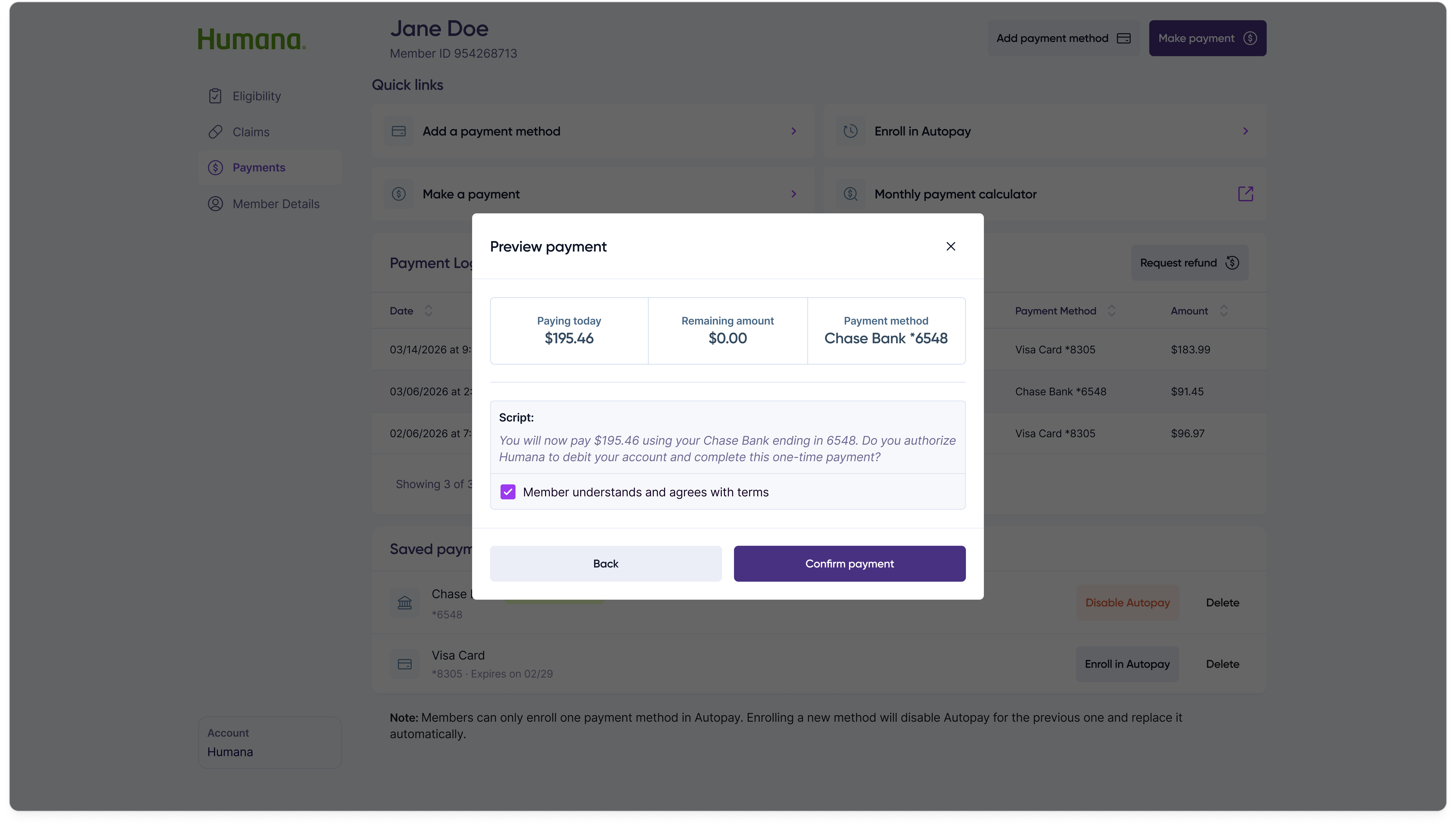
Step 4 — Confirmation
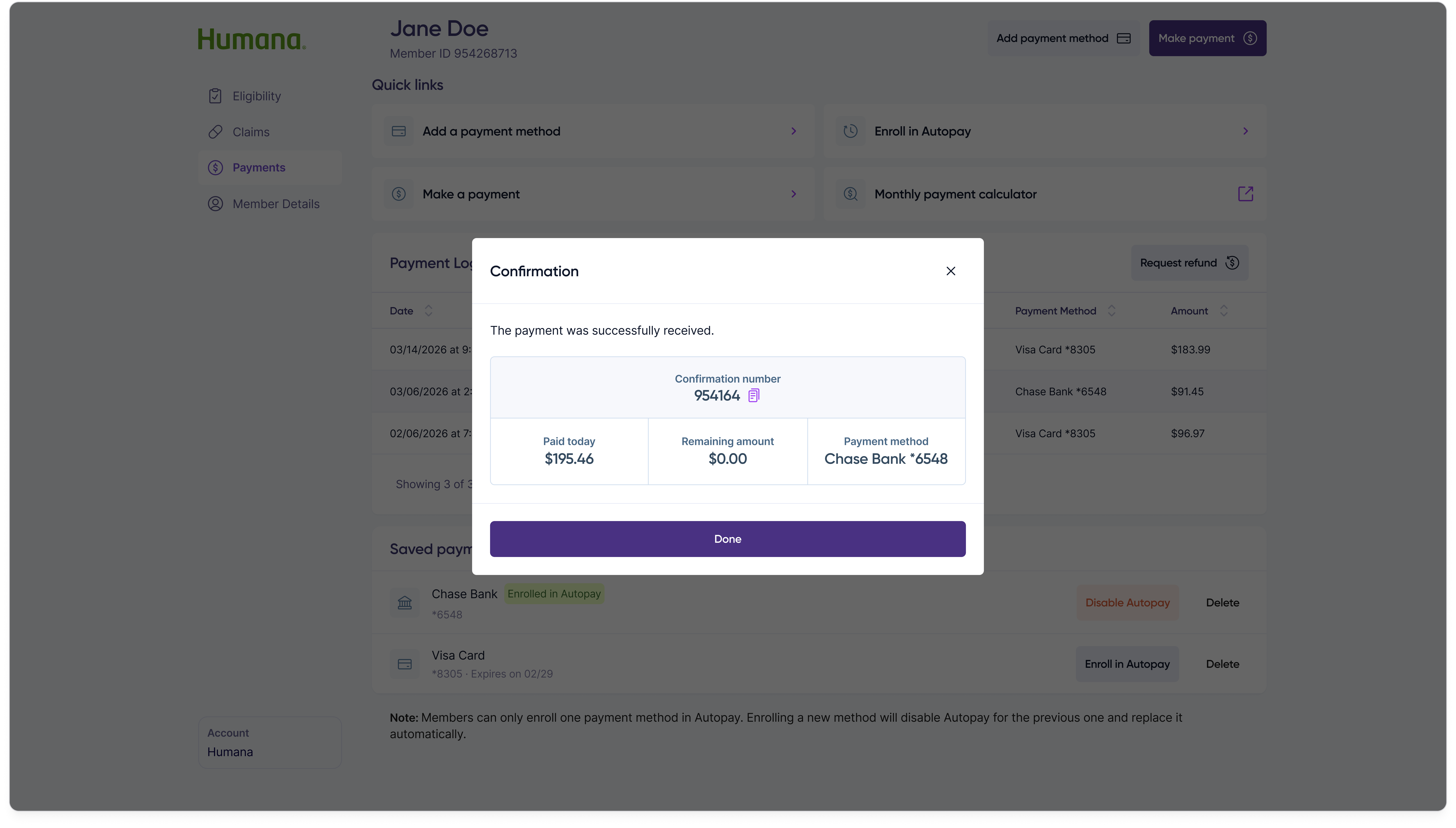
For members who don't want to remember a monthly call, customer reps can enroll a saved payment method into Autopay from the same Payments tab.
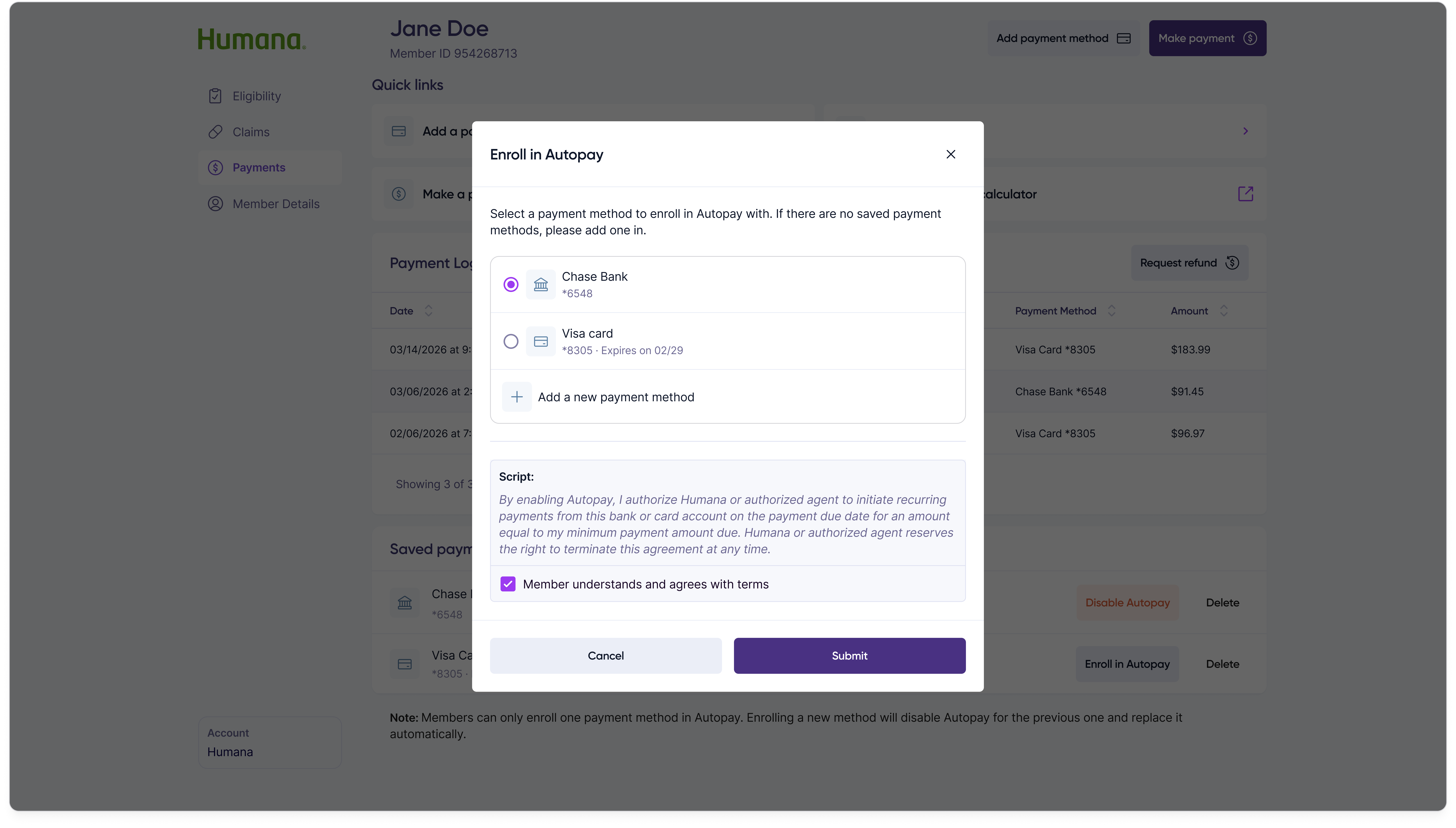
Result
The Medicare Prescription Payment Plan launched in October 2024 and is now available to 20M+ members (40% of the entire Medicare population) through Humana, Cigna, and Express Scripts.
10K+
Customer reps used this new portal to support members monthly.
$10M+
Revenue products from this product (~33% of total company revenue).
$83M+
In total managed balances.
20M+
Eligible members were able to opt-in and use this new program.